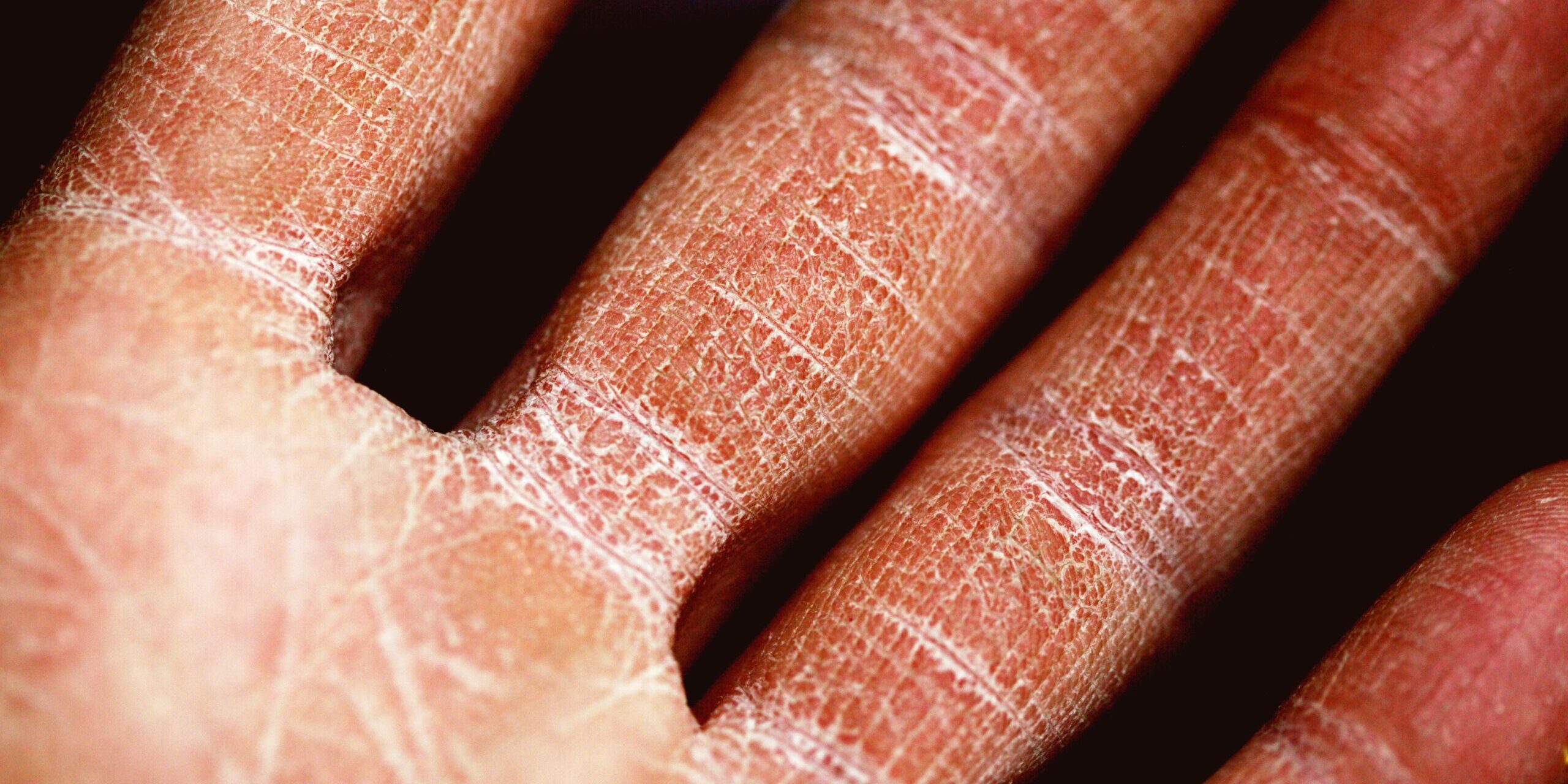
10 CAUSES OF ECZEMA THAT NOBODY TOLD YOU ABOUT
Eczema is a widespread skin condition that in the UK affects over 15 million people. It is characterised by itchy, red and scaly patches that can cover any part of the body and can be acute of chronic. It can develop an oozing crust that could get infected with a bacterium called staphylococcus aureus.
It is important to differentiate between different types of eczema: the first and most common is atopic eczema, which usually starts in childhood and is associated with other atopic conditions, the second is contact dermatitis, caused by a reaction to a substance that comes in contact with the area affected, the third is dyshidrotic eczema, characterised by blisters in hands and feet, the fourth is nummular eczema, where round shaped itchy spots appear on the skin, and the last one is stasis dermatitis, where fluid from the veins leaks out and causes swelling. Here we will just cover atopic dermatitis because is the most common.
 Within the atopic eczema we can have two further distinctions, the extrinsic, more common and IgE mediated (which means that is driven by allergies), and the intrinsic, non IgE mediated. They both have a similar clinical presentation.
Within the atopic eczema we can have two further distinctions, the extrinsic, more common and IgE mediated (which means that is driven by allergies), and the intrinsic, non IgE mediated. They both have a similar clinical presentation.
Now, let’s dive into the causes, which can be multifactorial and sometimes not easy to pinpoint.
- GENETICS. A variation on the filaggrin gene relates to skin barrier dysfunction. Filaggrin is a protein involved in epithelial cell differentiation, regulating the response to allergens and microbes, thus protecting the skin and preventing water loss. Interestingly, just 40% of individuals with this variation end up developing eczema, hence it must not be the only cause.
- ENVIRONMENT (AKA THE HYGIENE HYPOTESIS). There seems to be a correlation between poor exposure to pathogens and the incidence of eczema. Children like to play with all sorts of things and material, often putting in their mouth a vast array of non-edible items. This behaviour exposes them to various microbes and pathogens that strengthen their immune system. When we overclean our homes and don’t let the children play outside and get dirty, we deprive them of this opportunity.
- FAMILY HISTORY. There is a strong correlation between family history of atopic conditions like eczema, asthma and allergic rhinitis, and the incidence of eczema in the future generations. If one or both parents have any of the forementioned atopic condition, there is a high chance for their children to develop eczema.
- ALLERGIES. A good proportion of individuals with eczema (20-80%) has an IgE reaction to one or more foods, airborne allergens (like dust mite and animal dander), or topical products (particularly artificial fragrance, propylene glycol and lanolin). For each individual can be a completely different allergen, hence it is vital to recognise it via skin prick testing, elimination diet, blood test or patch test. The most common food allergy is gluten, followed by milk, peanuts and eggs.
- CHEMICAL EXPOSURE. Continuous exposure to some chemicals might trigger or drive eczema in some individuals. Chemicals used in hairdressing jobs, healthcare, bakeries and cleaning have a higher incidence in the development of eczema compared to other jobs with less chemical exposure.
- LOW VITAMIN D. Because of its pivotal role in immunity, low levels of vitamin D seems to be correlated to higher eczema prevalence. Vitamin D also contributes to healthy skin barrier function, preventing water loss and skin infections. The mechanisms behind it, however, are still not fully understood. Interestingly, skin exposure to ultraviolet light is used as adjunctive treatment for eczema.
- GUT DYSBIOSIS. When the gut is balanced, we have a symbiotic presence of different species of microbes. A 2019 study found that in the faeces of children with eczema there was a consistent lower number of some of those species (Bifidobacterium, Firmicutes, Bacteroides and Faecalibacterium) compared to the control group. Another study found that when there is a gut flora imbalance, some intestinal bacteria and their metabolites can travel through the bloodstream and accumulate in the skin where they trigger Th2 response. To confirm this hypothesis, a 2010 study found a correlation between early exposure to broad spectrum antibiotic and the risk of developing eczema as nearly three times higher compared to no antibiotic. Other gut conditions linked to AE as drivers and risk factors, are intestinal permeability and small intestinal bacterial overgrowth (SIBO).
- OBESITY. Recently, research has been investigating the correlation between eczema and obesity/overweight. There seem to be a weak association with moderate eczema but not with severe cases. No mechanism has been yet discovered, therefore more research is needed.
- ATOPIC MARCH. If an individual suffer from an atopic condition, then is more likely to develop asthma, eczema and allergic rhinitis progressively later in life. This is called atopic march, and it is usually characterised by an increase in severity of symptoms.
- HISTAMINE SENSITIVITY. Histamine is involved in inflammation, itchiness, skin’s tight junction integrity and skin barrier function. Histamine inhibits keratinocytes differentiation by reducing filaggrin expression, which result in the thinning of epidermis. Histamine can also disrupt tight junctions in endothelial and epithelial cells by suppressing intracellular junction proteins and desmosome components, although the exact mechanism is still unclear.
There are many potential causes for eczema, including genetic and allergies. It is particularly important to identify them in order to prevent flare ups. Speak to your doctor if you suspect a skin infection or if your current treatment no longer works.
REFERENCES
Brown, S. J. (2016). ‘Atopic eczema’. Clinical medicine, 16 (1), pp.66–69.
De Benedetto, A., Yoshida, T., Fridy, S. et al. (2015). ‘Histamine and Skin Barrier: Are Histamine Antagonists Useful for the Prevention or Treatment of Atopic Dermatitis?’. Journal of clinical medicine, 4 (4), pp.741–755.
Dhar, S., & Srinivas, S. M. (2016). Food Allergy in Atopic Dermatitis. Indian journal of dermatology, 61 (6), pp.645–648.
Hahn, E. Bacharier, L. (2005). ‘The atopic march: the pattern of allergic disease development in childhood’. Immunology and allergy clinics of North America, 25 (2), pp.231-246.
Kuo, I. H., Carpenter-Mendini, A., Yoshida, T. et al. (2013). ‘Activation of epidermal toll-like receptor 2 enhances tight junction function: implications for atopic dermatitis and skin barrier repair’. The Journal of investigative dermatology, 133 (4), pp.988–998.
Peters, A. S. Kellenberg, J. Vogelberg, C. et al. (2010). ‘Prediction of the incidence, recurrence, and persistence of atopic dermatitis in adolescence: A prospective cohort study’. The Journal of Allergy and Clinical Immunology, 126 (3), pp.590-595.
Schmitt, J. Schmitt, N. M. Kirch, W. et al. (2010). ‘Early exposure to antibiotics and infections and the incidence of atopic eczema: a population-based cohort study’. Paediatric allergy and immunology, 21 (2), pp.292-300.
Watanabe, S. Narisawa, Y. Arase, S. et al. (2003). ‘Differences in faecal microflora between patients with atopic dermatitis and healthy control subjects’. Journal of Allergy and clinical Immunology 111 (3), pp.587-591.
Zhang, A. Silverberg, J. I. (2015). ‘Association of atopic dermatitis with being overweight and obese: a systematic review and meta-analysis’. Journal of the American Academy of Dermatology 72 (4), pp.606-616.